Its main
steps are:
(1) Stimulation by Thyroid
Stimulating Hormone (TSH) secreted by the pituitary gland
(2) Iodide transported
from the blood stream to the follicular lumen -
iodide is concentrated to about 30 times blood
concentration via the Sodium/iodide pump (NIS)
(3) Thyroglobulin (Tg)
is produced and secreted inside the thyroid follicular
cell stimulated by TSH - and then Tg travels to the follicular lumen where
it is used to form thyroid hormones
(4) Iodide is oxidized to
iodine - via the thyroperoxidase enzyme (TPO) and mediated by
Hydrogen Peroxide (H2O2)
(5)
Tg undergoes iodination / Iodine is organified
()
for the production of iodotyrosines - also
catalysed by TPO, Iodine is incorporated
into tyrosine residues in theTg molecule and formed into iodotyrosines MIT and DIT
(thyroid hormone intermediates)
(6) Formation and storage
of Thyroid Hormones in Follicle Colloid - MIT and DIT (products of Tg
iodination) are bonded
via TPO to make the thyroid hormones T3 and T4, where they can be stored
for up to 3 months in the colloid of the follicular lumen, as part of thyroglobulin.
This storage form is called follicle colloid.
• MIT + DIT → T3 (3 iodides)
Via TPO
• DIT + DIT→ T4
(4 iodides) Via TPO
(7) When needed, TSH stimulates
release of T3 and T4 - thyroid hormones are reabsorbed from the colloid in
the follicular lumen into the follicular cells, where they are cleaved from thyroglobulin
(Tg) and released into circulation
Importance of appropriate iodine supply for making thyroid
hormones
- Too much
or too little iodine impairs adequate TH synthesis - as at any factory, effective
production depends on three key components - adequate raw material (T4 is
65% iodine by weight), efficient machinery, and appropriate controls.
Like many things in life, the amount of iodine
required for a smooth operation has a "Goldilocks" factor - too much or too little
available iodine detrimentally affects the auto-regulation of T3 / T4 synthesis,
and in either case can cause goiter (a swollen thyroid gland).
For more detailed information on thyroid hormone production:
Thyroid Hormone
Production - In detail
Thyroid Production
Feedback Loop
Thyroid's T4/T3 production is controlled
by hypothalamic control of the pituitary gland's production of thyroid stimulating
hormone (TSH), by negative feedback of T3/T4 levels
The hypothalamus in the brain releases TRH
(Thyrotropin-Releasing Hormone) - to modulate the
pituitary gland's release of TSH (Thyroid Stimulating
Hormone);
TSH circulating in the bloodstream tells the thyroid
to make T3 and T4 thyroid hormones - and release them into the bloodstream,
to be converted as needed to T3, mainly by the liver;

The pituitary gland's TSH production is sensitive to the T3/T4
levels in the blood
- When the
T3/T4 levels drop, the pituitary produces and releases more TSH - to
stimulate the thyroid to make more T4 and T3 thyroid hormones and release them into
the bloodstream;
- As the
thyroid hormone levels rise, the pituitary reduces or shuts off TSH - This
negative feedback mechanism keeps the level of thyroid hormones in
a fairly constant range with a normally-functioning thyroid.
TSH production is also reduced by:
-
Somatostatin - hormone that inhibits secretion of growth hormone
-
Rising levels of glucocorticoids and sex hormones (e.g.
Estrogen,
TESTOSTERONE)
- Excessively high blood
iodide
concentration - as a self protecting mechanism.
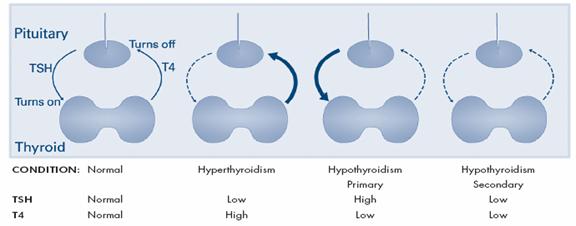
TSH-T4 level conditions
- Stress
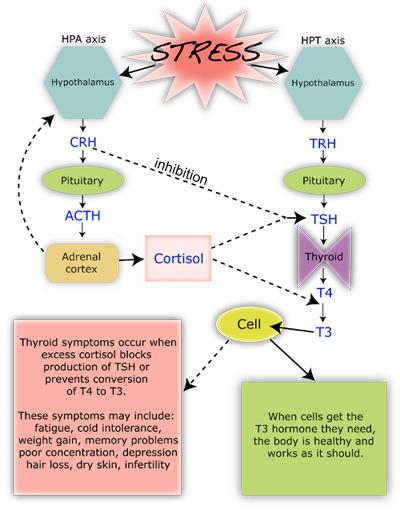
Stress Affects TH production
and T4 to T3 Conversion
Neither TSH
or blood Plasma T3/T4 Levels alone are a substantive evaluation of thyroid function
The level of thyroid hormone
(i.e. T3 and T4) production is determined
by:
- Levels
of TSH released from the pituitary gland - producing a feedback loop so that
TSH increases as thyroid hormones decrease, and TSH decreases when thyroid hormones
increase;
- AVAILABILITY
of IODINE
and TYROSINE(converted by the thyroid to the thyroid
hormones) - Insufficient iodine
causes thyroid cell enlargement (hypertrophy), leading to an enlarged thyroid (goiter).
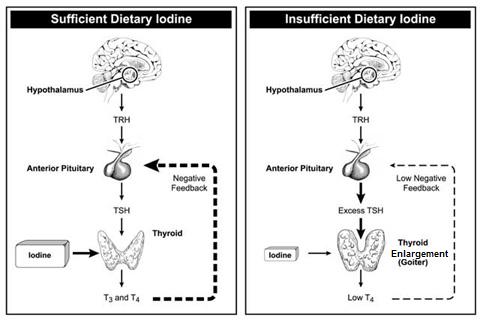
Iodine Availability
- The condition
of the thyroid tissues themselves;
-
Further regulated by the hypothalamus, by other nutrient requirements, and
no doubt other regulatory mechanisms;
-
TSH level is also not a reliable indicator of thyroid function for many people
(E.g. Low amounts of
T4 in the blood, due to lack of dietary
iodine to make them,
gives rise to high levels of TSH);

