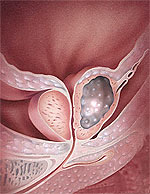
The prostate gland. The purpose of the prostate gland is to produce fluid to nourish sperm and stimulate their motility. Prostatic fluid makes up about 1/3 of semen.
Prostate cancer is usually a slow-growing carcinoma (cancer of epithelium / lining) in the prostate gland. Cancer typically forms in the prostate's glandular tissue, doubling in size every 4-5 years, but sometimes it is in the prostate muscle and connective tissue. Initially cancer cells are confined to the prostate, present no symptoms and cause no harm, but in time they can metastasize (usually to bones or lymph nodes), at which time symptoms present and the risk of dying is significantly increased. That said, a man may have PC without even being aware of it - and in fact, almost 80% of men over 80 yrs who die of other causes have PC.
Some types of PC can be more aggressive - presenting symptoms earlier than usual that may require treatment.
Prostate enlargement (Benign Prostate Hyperplasia or BPH - a major cause of problems in older men) may be associated with prostate cancer.
Prostate cancer is the second-most commonly diagnosed cancer in American men (after skin cancer)
Probability of getting prostate cancer increases with age - mostly affecting males over age 50. About 6 out of 10 cases diagnosed are in men aged 65 or older, and it is rare before age 40. The average age at the time of diagnosis is about 66.
Prostate cancer incidence and mortality rates are significantly higher in the Western world compared to Asian populations - suggesting a possible dietary / environmental link. (statistics are age-standardized to give a better comparison since PC is predominant in older men).
Usually detected by a high Prostate Specific Antigen (PSA) count (although there are other tests more indicative of prostate cancer and its progress) - the PSA count is higher when the immune system is dealing with a prostate problem. A slightly raised PSA count could simply be due to an infection / inflammation of the prostate. A normal PSA level is less than 4 ng / mL of blood. 4-10 ng / mL suggests possible BPH or prostate cancer (in 25% of men), over 10 ng / mL is associated with prostate cancer (in 50% of men). Men in their 50's or younger typically have a PSA around 2.5 ng / mL. PSA readings have no upper limit and can reach 10,000 ng / mL or more.
Ultra-scans and prostate biopsies. Cancer tumors are typically found here and there throughout the prostate, and not as a single prostate cancer mass.
Overlapping symptoms of prostate enlargement (benign prostate hyperplasia / BPH) and prostate cancer sometimes make it difficult to distinguish between the two:
However, there are some distinct symptoms signifying prostate cancer vs. benign prostate hyperplasia (BPH / Enlarged prostate):
Age. Your risk of prostate cancer increases as you age.
Obesity. Waist circumference / belly fat increases your risk of dying early. Each 4 in.of waist size increases the chance of developing fatal PC by 18% and a premature death from any cause by 11%., according to an Oxford university study (published in 2020) involving 140,000 men, mean age 52 years, across 8 countries. The study also found that obesity increased the risk of getting a high-grade (aggressive form) of PC by 13%. University of Oxford Study published in the British Medical Journal, 2020

Race.
Family history. If men in your family have had prostate cancer, your risk may be increased. Also, if you have a family history of genes that increase the risk of breast cancer (BRCA1 or BRCA2) or a very strong family history of breast cancer, your risk of prostate cancer may be higher. Familial prostate cancer occurs in about 10% of cases - occurring at an earlier age than non- familal prostate cancer. World Health Organization: Cancers of the male reproductive tract. In World Cancer Report, Stewart BW and Kleihues P (eds). Lyon, France: IARC Press, 2003, pp 208- 211.
Vitamin K2 deficiency
Fat intake. Urinary concentrations of androgens and estrogens decreased in a group of white and black men who had decreased their dietary fat intake.74
Magnesium Deficiency / Calcium Excess
The main hormones involved in prostate cancer
Mainstream medicine focuses on high level testosterone as the main culprit in PC. However, there is a lack of credible evidence from many studies looking for a correlation between testosterone levels and PC occurrence;
Androgen-deprivation treatment (ADT) decreases life expectancy by causing heart disease:
DHT is more the problem than testosterone
Males produce progesterone (~ 1/2 the amount of women) which prevents the body's conversion of testosterone to DHT by inhibiting the enzyme 5-alpha reductase (even more effectively than Proscar and Saw Palmetto - the often-used agents used in traditional and natural medicine).
Cancer-protective gene p53 / Cancer-causing BCL2 oncogene |
|
All cells (except brain and muscle cells) multiply continuously, with cell growth regulated by the p53 and bcl-2 genes
One way to cure cancer is to find agents that activate p53 and deactivate bcl-2:
|
Dr. John R. Lee (a pioneer of natural hormone therapy) hypothesizes that estrogen dominance over testosterone is a more probable cause than high testosterone levels - referencing estrogen dominance as the only known cause of uterine cancer (where, in women, estrogen is dominant over progesterone), he mentions that both the uterus and prostate develop from the same embryonic cells, and both contain the oncogene BCL- 2 (B- cell lymphoma 2), and the cancer protective gene P53
Estradiol increases cell proliferation, progesterone decreases it
P53 gene "tells" cell to die on time by promoting its apoptosis (or natural cell death) and can also stop DNA-damaged cells from dividing. If p53 gene dominates, the products of this gene activation promote healthy apoptosis, and thus control cell growth, such that cancer does not occur.
Bcl-2 gene blocks the p53 cancer- protective gene. If bcl-2 dominates, cell growth increases, i.e. cells become cancerous.
In 1997, Dr.T.S. Wiley and Dr. Ben Formby (a Danish molecular biologist) grew cell cultures of breast, endometrium, ovary and prostate. Adding estradiol turned on the bcl-2 gene resulting in cells growing rapidly and not dying. By next adding progesterone, the cells stopped growing as rapidly, died on time and the cancer disappeared. 1997, Dr.T.S. Wiley and Dr. Ben Formby, U. of California, Santa Barbara
To summarize - Contrary to mainstream belief, it is the estrogen estradiol that causes prostate cancer, not testosterone. In men, if the estradiol to testosterone ratio changes to cause a dominance of estradiol, prostate cancer cells can develop. However, testosterone must also be present for prostate cancer to occur. Progesterone supplementation is an obvious treatment for men with testosterone deficiency relative to their estradiol levels.
McConnell JD. Benign prostatic hyperplasia: diagnosis and treatment. Benign Prostatic Hyperplasia Guideline Panel. Rockville, Md.: U.S. Dept. of Health and Human Services, Public Health Service, Agency for Health Care Policy and Research, 1994; Clinical practice guideline no. 8, AHCPR publication no. 94–0582.
Austin O, Ricer RE. Prostate cancer screening: an appraisal of the PSA test. Fam Pract Recert. 1996;18:81-91.